11 results
Antidepressants overuse in primary care: prescription trends between 2010-2019 in Catalonia
- M. S. Gonzalez, G. anmella, E. vieta, M. Primé-Tous, X. Segú, A. Mas, D. Hidalgo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S545
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Antidepressants (AD) are one of the most prescribed pharmacological treatments in developed countries. AD efficacy is well-proven in anxiety, depressive and other mental disorders, but their use is also common in individuals without psychiatric health conditions. Indeed, recent evidence reported an increase in AD prescription over the latest years. Concern has been raised on the overuse of AD in several countries, and societal policies and national guidelines have been developed to regulate their use in the general population.
Several factor might be used to explain this increase, including the more safety profile of new AD classes (i.e. SSRI, or vortioxetine) compared to old AD, a possible overall increase in the incidence of depressive and anxiety disorders, or their inappropriate prescription in mild conditions which could be managed without pharmacological treatment as first-step option in primary care (PC).
ObjectivesExplore AD prescription patterns in relation to mental health diagnoses and identify the most relevant factors involved in PC health systems. Understanding the variables influencing AD prescription would allow designing strategies and guidelines to make appropriate use of this pharmacological group in PC. As part of the PRESTO project (www.prestoclinic.cat), here we investigated the changes in frequency and the variables associated with AD prescription in a population-representative sample of people attending PC between 2010 –2019 in Catalonia, Spain.
MethodsWe retrieved AD prescription, sociodemographic, and health-related data using individual electronic health records from a population-representative sample (N=947.698) attending PC between 2010-2019. Prescription of AD was calculated using DHD (Defined Daily Doses per 1,000 inhabitants/day). We compared cumulative changes in DHD with cumulative changes in diagnoses with an indication for AD during the study period. We used Poisson regression to examine sociodemographic and health-related variables associated with AD prescription.
ResultsBoth AD prescription and mental health diagnoses with an indication for AD gradually increased. At the end of the study period, DHD of AD prescriptions and mental health diagnoses with an indication for AD reached cumulative increases of 404% and 49% respectively. Female sex (incidence rate ratio (IRR)= 2.83), older age (IRR = 25.43), and lower socio-economic status (IRR= 1.35) were significantly associated with increased risk of being prescribed an AD.
ConclusionsOur results from a large and representative cohort of patients confirm a steady increase of AD prescriptions that is not explained by a parallel increase in mental health diagnoses with an indication for AD. A trend on AD off-label and over-prescriptions in the PC system in Catalonia can be inferred from this dissociation.
Disclosure of InterestM. Gonzalez: None Declared, G. anmella Grant / Research support from: received CME-related honoraria, or consulting fees from Janssen-Cilag, Lundbeck, Lundbeck/Otsuka, and Angelini, with no financial or other relationship relevant to the subject of this article, E. vieta Grant / Research support from: received research support from or served as consultant, adviser or speaker for AB-Biotics, Abbott, Abbvie, Adamed, Angelini, Biogen, Celon, Dainippon Sumitomo Pharma, Ferrer, Gedeon Richter, GH Research, Glaxo SmithKline, Janssen, Lundbeck, Organon, Otsuka, Rovi, Sage pharmaceuticals, Sanofi-Aventis, Shire, Sunovion, Takeda, and Viatris, out of the submitted work, M. Primé-Tous: None Declared, X. Segú: None Declared, A. Mas: None Declared, D. Hidalgo Grant / Research support from: received CME-related honoraria or adviser from Abbott, Angelini, Janssen-Cilag and Ethypharm with no financial or other relationship relevant to the subject of this article.
Meta-analysis of the variability in the individual response to pharmacological treatments for mania in bipolar disorder
- G. Anmella, M. De Prisco, V. Oliva, M. Sanabra, L. Fortea, M. Ortuño, G. Fico, A. Murru, E. Vieta, D. Hidalgo-Mazzei, A. Solanes, J. Radua
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S84
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Many studies have investigated whether there exist predictors of good response to antimanic drugs in bipolar disorder (BD). However, these factors predict response or only indicate benign illness course.
ObjectivesTo shed some light on the topic, we tested whether the response to antimanic drugs showed any variability beyond that expected by the effects of illness course and placebo.
MethodsWe included all double-blind, placebo-controlled RCTs of oral pharmacotherapies targeting adult patients with acute bipolar mania from 1991 to 2020. The primary outcome was the variance of the improvement in manic symptoms in treated individuals compared to placebo. The effect size was the log variability ratio (logVR). We performed a random-effects meta-analysis, including assessments of heterogeneity, sensitivity/cumulative/subgroup analyses, and meta-regression.
Results42 RCTs (46 comparisons) from a total of 8,438 BD patients with acute mania (53.7% male, mean age=39.3; 5,563 treatment/2,875 control groups) were included in the analysis. Individuals in active treatment groups did not show variability in the response beyond that observed in individuals under placebo (VR=1; 95% C.I.=0.97,1.03; p-value=0.97). No heterogeneity was detected between the studies (I2=0%; tau2=0%; Q=29.21; df=45; p-value=0.97). Results were similar in the leave-one-out/cumulative/subgroup analyses. Meta-regression did not show influences by age, sample size, sex, severity of manic symptoms at baseline, or clinical features (rapid cycling, mixed or psychotic features).
ConclusionsThis meta-analysis shows no evidence of differences in the individual response to treatments. These findings suggest that the average treatment effect is a reasonable assumption for the individual BD patient with acute mania. The presented article adds evidence to the equivalent results in schizophrenia-spectrum disorders, clinical high-risk state for psychosis, and major depressive disorder, not supporting classification in responders vs. non-responders. However, these findings should be balanced with results from other fields supporting such classification.
Disclosure of InterestNone Declared
Does bipolar disorder differ from other mental illnesses in terms of emotion dysregulation? A systematic review and meta-analysis
- M. De Prisco, V. Oliva, G. Fico, J. Radua, I. Grande, N. Roberto, G. Anmella, D. Hidalgo-Mazzei, M. Fornaro, A. de Bartolomeis, A. Serretti, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S571-S572
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Emotion regulation (ER) is the ability to assess, monitor, or modify emotional reactions to achieve a goal (Gross. Psychological inquiry 2015; 26 1-26). When ER strategies are rigidly or maladaptively applied, emotional dysregulation (ED) can occur (Thompson. Development and psychopathology 2019; 31 805-815). ED is common in people diagnosed with bipolar disorder (BD), but it can also be described in other clinical populations given its transdiagnostic nature. Numerous aspects of ED have been described in BD (De Prisco et al. Neuroscience & Biobehavioral Reviews 2022; 104914), but it is unclear whether these manifest similarly in other conditions such as major depressive disorder (MDD) or borderline personality disorder (BPD), or whether they are specific to BD.
ObjectivesThe objective of this systematic review and meta-analysis is to examine the literature comparing BD with other psychiatric disorders in terms of ED, focusing on those studies using validated clinical tools.
MethodsA systematic search from inception to April 28th, 2022, was conducted exploring the PubMed/MEDLINE,EMBASE, Scopus, and PsycINFO databases. Those studies providing quantitative data on ED in people diagnosed with BD and compared with clinical groups were eligible for inclusion. No restriction about age, sample size, or language were applied. Random effect meta-analyses were conducted, and effect sizes were calculated as standardized mean differences (SMD).
ResultsA total of 3,239 records was identified and, after duplicate removal and title/abstract evaluation, 112 were explored at the full text. Twenty-nine studies were finally included, and it was possible to perform a meta-analysis with twenty-two (145 comparisons) of them. Only studies comparing BD with MDD, and BPD provided sufficient data to perform a meta-analysis. People with BD did not differ from people with MDD in most of the comparisons considered. However, BD patients presented higher positive rumination (two comparisons: SMD=0.46; CI=0.27, 0.64; p=8.5e-07; I2=0%; and SMD=0.34; CI=0.15, 0.52; p=2.7e-04; I2=0%) and risk-taking behaviors (SMD=0.48; CI=0.27, 0.69; p=8.11e-06; I2=0%). In contrast, people with BPD displayed an overall higher degree of ED (SMD=-1.22; CI=-1.94, -0.5; p=9.1e-04; I2= 90.7) and used fewer adaptive ER strategies. Additionally, higher levels of self-blaming (SMD=-0.80; CI=-1.11, -0.50; p=2.68e-07; I2=0) and impulsive behavior (SMD=-0.76; CI=-0.89, -0.63; p=5.4e-29; I2=0) were observed.
Image:
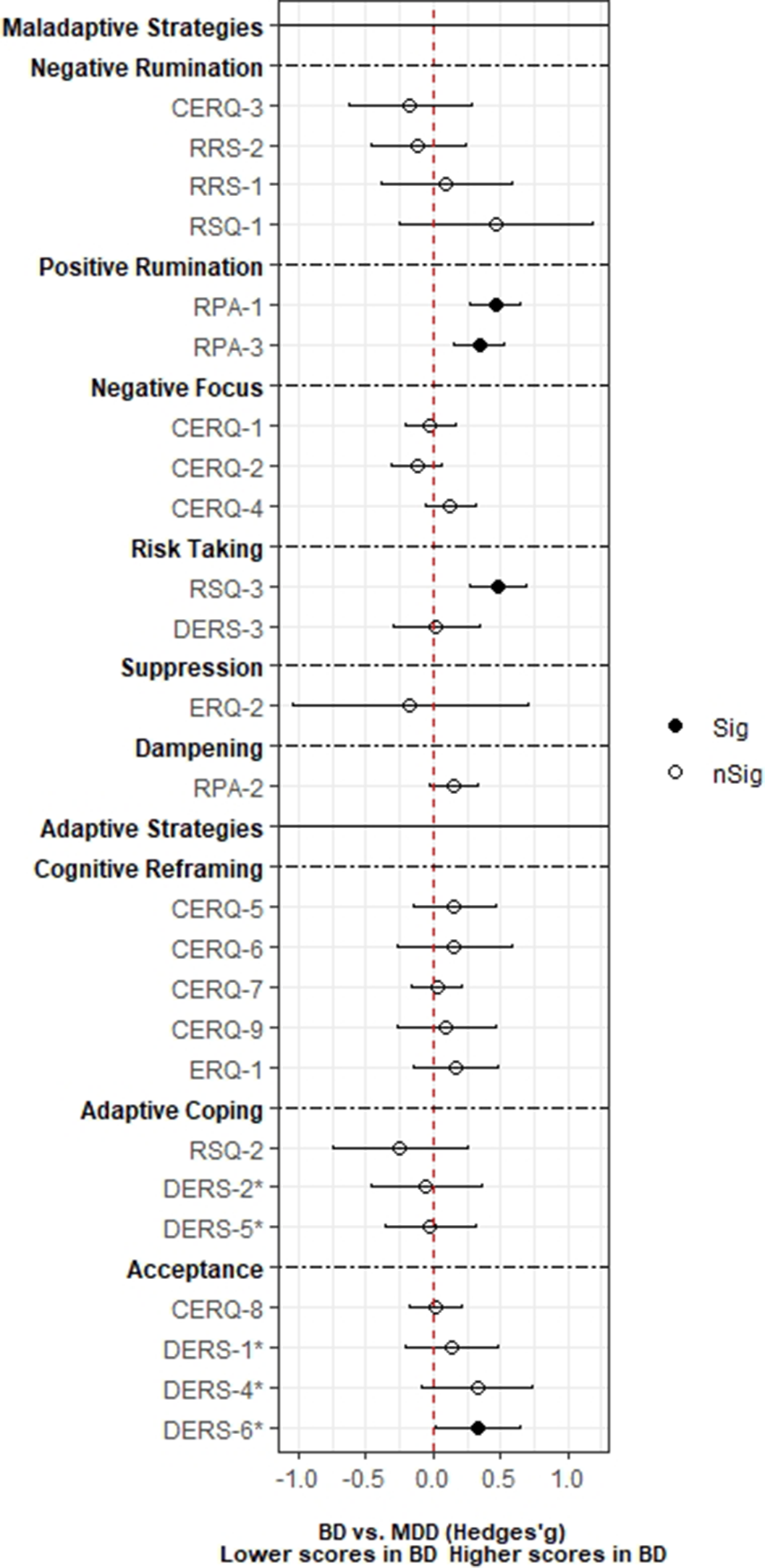
Image 2:
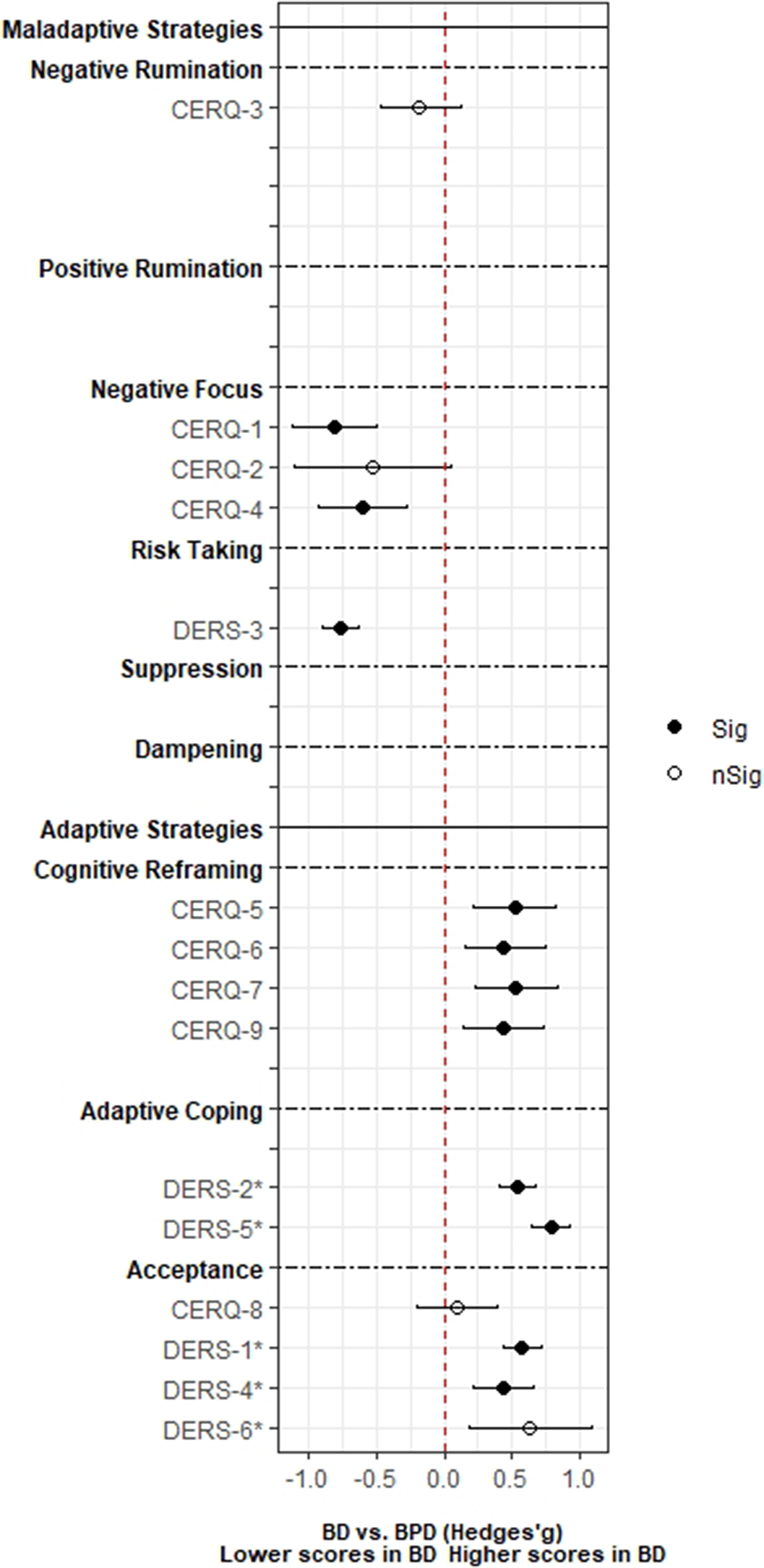 Conclusions
ConclusionsED is a trans-diagnostic construct that spans a continuum of different psychiatric disorders. Outlining the specific clinical features of one disorder versus another may help future research to increase our knowledge of these issues and develop new treatment strategies to reduce the clinical burden of these patients.
Disclosure of InterestM. De Prisco: None Declared, V. Oliva: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, I. Grande Grant / Research support from: Spanish Ministry of Science and Innovation (MCIN) (PI19/00954) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII-Subdirección General de Evaluación y el Fondos Europeos de la Unión Europea (FEDER, FSE, Next Generation EU/Plan de Recuperación Transformación y Resiliencia_PRTR ); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); and the the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), CERCA Programme / Generalitat de Catalunya as well as the Fundació Clínic per la Recerca Biomèdica (Pons Bartran 2022-FRCB_PB1_2022), Consultant of: ADAMED, Angelini, Casen Recordati, Ferrer, Janssen Cilag, and Lundbeck, Lundbeck-Otsuka, Luye, SEI Healthcare, N. Roberto: None Declared, G. Anmella Grant / Research support from: Rio Hortega 2021 grant (CM21/00017) from the Spanish Ministry of Health financed by the Instituto de Salud Carlos III (ISCIII) and co-financed by the Fondo Social Europeo Plus (FSE+), Consultant of: Janssen-Cilag, Lundbeck, Lundbeck/Otsuka, and Angelini, D. Hidalgo-Mazzei Grant / Research support from: Juan Rodés JR18/00021 granted by the Instituto de Salud Carlos III (ISCIII), M. Fornaro: None Declared, A. de Bartolomeis Consultant of: Janssen, Lundbeck, and Otsuka and lecture fees for educational meeting from Chiesi, Lundbeck, Roche, Sunovion, Vitria, Recordati, Angelini and Takeda; he has served on advisory boards for Eli Lilly, Jansen, Lundbeck, Otsuka, Roche, and Takeda, Chiesi, Recordati, Angelini, Vitria, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda
Vickybot, a chatbot for anxiety-depressive symptoms and work-related burnout
- G. Anmella, M. Sanabra, M. Primé-tous, X. Segú, M. Cavero, R. Navinés, A. Mas, V. Olivé, L. Pujol, S. Quesada, C. Pio, M. Villegas, I. Grande, I. Morilla, A. Martínez-Aran, V. Ruiz, E. Vieta, D. Hidalgo-Mazzei
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S109-S110
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A significant proportion of people attending Primary Care (PC) have anxiety-depressive symptoms and work-related burnout and there is a lack of resources to attend them. The COVID-19 pandemic has worsened this problem, particularly affecting healthcare workers, and digital tools have been proposed as a workaround.
ObjectivesWe present the development, feasibility and effectiveness studies of chatbot (Vickybot) aimed at screening, monitoring, and reducing anxiety-depressive symptoms and work-related burnout in PC patients and healthcare workers.
MethodsUser-centered development strategies were adopted. Main functions included self-assessments, psychological modules, and emergency alerts. (1) Simulation: HCs used Vickybot for 2 weeks to simulate different possible clinical situations and evaluated their experience. (3) Feasibility and effectiveness study: People consulting PC or healthcare workers with mental health problems were offered to use Vickybot for one month. Self-assessments for anxiety (GAD-7) and depression (PHQ-9) symptoms, and work-related burnout (based on the Maslach Burnout Inventory) were administered at baseline and every two weeks. Feasibility was determined based on the combination of both subjective and objective user-engagement Indicators (UEIs). Effectiveness was measured using paired t-tests as the change in self-assessment scores.
Results(1) Simulation: 17 HCs (73% female; mean age=36.5±9.7) simulated different clinical situations. 98.8% of the expected modules were recommended according to each simulation. Suicidal alerts were correctly activated and received by the research team. (2) Feasibility and effectiveness study: 34 patients (15 from PC and 19 healthcare workers; 77% female; mean age=35.3±10.1) completed the first self-assessments, with 34 (100%) presenting anxiety symptoms, 32 (94%) depressive symptoms, and 22 (64.7%) work-related burnout. Nine (26.5%) patients completed the second self-assessments after 2-weeks of use. No significant differences were found for anxiety [t(8) = 1.000, p = 0.347] or depressive [t(8) = 0.400, p = 0.700] symptoms, but work-related burnout was significantly reduced [t(8) = 2.874, p = 0.021] between the means of the first and second self-assessments. Vickybot showed high subjective-UEIs, but low objective-UEIs (completion, adherence, compliance, and engagement).
ConclusionsThe chatbot proved to be useful in screening the presence and severity of anxiety and depressive symptoms, in reducing work-related burnout, and in detecting suicidal risk. Subjective perceptions of use contrasted with low objective-use metrics. Our results are promising, but suggest the need to adapt and enhance the smartphone-based solution in order to improve engagement. Consensus on how to report UEIs and validate digital solutions, especially for chatbots, are required.
Disclosure of InterestNone Declared
A family history of suicide in bipolar disorders: powerful, powerless
- M. Sagué Vilavella, G. Fico, G. Anmella, A. Giménez, M. Gómez Ramiro, M. T. Pons Cabrera, S. Madero, A. Murru, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S387
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
When completing the medical record of a patient with bipolar disoder (BD), hardly anything is more impacting than a family history of completed suicide (FHS). In fact, FHS is a main risk factor for personal suicide attempts and death in this population. There are few modifiable protective factors against suicide in BD, such as lithium treatment and absence of substance abuse.
ObjectivesWe aimed to explore the relationship between a FHS and clinical characteristics in patients with BD. Given the impact that FHS has on the individual and on healthcare professionals, we hypothesized that it would modify behaviors towards a higher prevalence of the modifiable protective factors against suicide, namely more treatment with lithium and less drug addiction.
MethodsThis is a cross-sectional study that included all patients with BD that were followed up in a specialised unit between 1998 and 2020. Only subjects with complete information on FHS were retained for the analysis. We assessed sociodemographic and clinical data and described it with measures of frequency, central tendency and dispersion. Differences between subjects with and without FHS were calculated with χ², Fisher’s exact test and Student’s t-test as appropriate. We set the significance level at p≤0.05. All tests were two-tailed.
ResultsThe sample consisted of 480 subjects with a mean age of 45.9 years (standard deviation 14.4, range 18-88), of which 54.4% (n=261) were women. 69.2% (n=332) had a diagnosis of BD type I and 30.8% (n=148) of BD type II. 77 subjects (16%) had a FHS. Regarding differences between groups, those with relatives who had committed suicide did not show statistically significant differences in terms of sociodemographic variables (age, gender, civil status, employment) or key clinical features (type of BD, illness duration, psychotic features, predominant polarity, rapid cycling, number of lifetime manic and depressive episodes, comorbid personality disorder), neither did they have a higher use of lithium (55.8% vs 59.3%, p=0.572) nor lower substance use disorder (10.9% vs 15.5%, p=0.34). Predictably, people with FHS had a higher prevalence of family history of mental and affective disorders (96.1% vs 70.9%, p<0.001; 86.3% vs 56.3%, p<0.001) and of stressful life events (71.6% vs 58.9%, p=0.05). Personal lifetime suicide attempts also tended to be higher (36.4% vs 26.7%, p=0.088).
ConclusionsContrary to our hypothesis, in our sample of subjects with BD a FHS was not associated with a higher prevalence of the modifiable protective factors against suicide. Therefore, although suicide has a major impact both in families and healthcare professionals, our results suggest it does not modify attitudes towards prevention in a real-life scenario. The main limitation of our study is its cross-sectional design, which does not allow for causal inference. In conclusion, there is room for improvement in the fight against suicide.
Disclosure of InterestNone Declared
The TIMEBASE Study: IdenTifying dIgital bioMarkers of illnEss activity in BipolAr diSordEr. Preliminary results
- G. Anmella, A. Mas, I. Pacchiarotti, T. Fernández, A. Bastidas, I. Agasi, M. Garriga, N. Verdolini, N. Arbelo, D. Nicolás, V. Ruiz, M. Valentí, A. Murru, E. Vieta, A. Solanes, F. Corponi, B. Li, D. Hidalgo-Mazzei
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S221
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mood episodes in bipolar disorder (BD) are still identified with subjective retrospective reports and scales. Digital biomarkers, such as actigraphy, heart rate variability, or ElectroDermal activity (EDA) have demonstrated their potential to objectively capture illness activity.
ObjectivesTo identify physiological digital signatures of illness activity during acute episodes of BD compared to euthymia and healthy controls (HC) using a novel wearable device (Empatica´s E4).
MethodsA pragmatic exploratory study. The sample will include 3 independent groups totalizing 60 individuals: 36 BD inpatients admitted due to severe acute episodes of mania (N=12), depression (N=12), and mixed features (N=12), will wear the E4-device at four timepoints: the acute phase (T0), treatment response (T1), symptoms remission (T2) and during euthymia (T3; outpatient follow-up). 12 BD euthymic outpatients and 12 HC will be asked to wear the E4-device once. Data pre-processing included average downsampling, channel time-alignment in 2D segments, 3D-array stacking of segments, and random shuffling for training/validation sets. Finally, machine learning algorithms will be applied.
ResultsA total of 10 patients and 5 HC have been recruited so far. The preliminary results follow the first differences between the physiological digital biomarkers between manic and depressive episodes. 3 fully connected layers with 32 hidden units, ectified linear activation function (ReLU) activation, 25% dropout rate, significantly differentiated a manic from a depressive episode at different timepoints (T0, T1, T2).
ConclusionsNew wearables technologies might provide objective decision-support parameters based on digital signatures of symptoms that would allow tailored treatments and early identification of symptoms.
DisclosureNo significant relationships.
Neutropenia induced by Valproic Acid: A case report
- N. Baldaquí, G. Anmella, S. Madero, F. Gutierrez, E. Pujal, L. Colomer, A. Giménez-Palomo
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S731-S732
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Valproic acid (VPA) is considered a well-tolerated antiepileptic drug used in Bipolar Disorder as a mood stabilizer. Nevertheless, VPA has been related to several adverse effects. Neutropenia is included as a potential adverse effect, although in clinical practice it is not often measured with regularity.
ObjectivesTo report a case of a patient with Bipolar Disorder type 2 and Personality Disorder Cluster B treated with VPA with a neutropenia caused by VPA.
MethodsA 61-year-old woman assists to the outpatient psychiatric unit in order to a pharmacological treatment adjustment. A blood test is performed showing a decrease in the levels of neutrophiles in comparison with previous tests. Psychiatric history is revised finding and association between the prescription of VPA and the reduction of neutrophile levels. When this drug was removed, neutrophile levels had increased again up to normal levels.
ResultsDue to the relationship between neutropenia and VPA treatment, we decided to discontinue this drug. At the beginning the patient doesn’t agree with the withdrawal of VPA treatment due to its effectiveness in her mood stabilization. Psychoeducation sessions are performed in order to explain risk and benefits of potentials treatment alternatives versus maintaining the same prescription. Finally the patient accepts the switch of the mood stabilizer treatment to oxcarbazepine with a good tolerability and effectiveness.
ConclusionsPeriodical blood test monitoring is needed in order to study adverse effects as neutropenia in patients with VPA treatment.
DisclosureThe author has received support from Janssen-Cilag, Otsuka-Lundbeck, Italfármaco, Angelini Pharma and Casen Recordati; and declares no support related to the subject of this article.
PRESTOapp for health workers with mental health symptoms related to the COVID-19 pandemic
- M. Primé Tous, G. Anmella, X. Segú, M.D.R. Fernández Canseco, C. Carrino, M. Villegas, V. Vicens, J. Blanch, M. Cavero, E. Vieta, D. Hidalgo-Mazzei
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S575
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The COVID-19 pandemic has caused a significant impact on the mental health of health workers that has brought many hospitals to launch immediate preventive mental health programs.
Objectives(1) To adapt and enhance a smartphone app (PRESTOapp) for health workers with mental health symptoms related to the COVID-19, and (2) to demonstrate its potential effectiveness in significantly reducing anxiety-depressive and PTSD symptoms in this population. We aim to incorporate Natural Language Processing (NLP)-based techniques in a chatbot user-interface that will enable a more personalized and accurate monitoring and intervention.
MethodsAn 18-months study with a 6-months preliminary phase to adapt PRESTOapp to health workers, enhance it with NLP-based techniques and chatbot user-interface, and evaluate its feasibility, and effectiveness in 12-months.
ResultsPRESTOapp has the potential to provide a prompt, personalized and integral response to the mental health demand due to the COVID-19. It will help by providing an innovative digital platform, that will allow remote monitoring of the symptoms course, provide brief psychotherapeutic interventions, and detect urgent situations. If the preliminary results of this study point to a potential effectiveness of the intervention, PRESTOapp may be easily adapted to the general population.
ConclusionsPRESTOapp may be one of the key digital platforms that may help preventing and treating potentially severe mental health consequences. Considering the unresolved problem of burnout in health workers even before the COVID-19, this project will develop the necessary technology for implementing cost-effective mental health solutions, not only during the pandemic.
DisclosureNo significant relationships.
Bipolar disorders and suicide: stumbling twice with the same stone?
- M. Sagué-Vilavella, G. Fico, G. Anmella, A. Giménez-Palomo, M. Gómez-Ramiro, M. Pons Cabrera, S. Madero, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S222-S223
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is the most terrible outcome of bipolar disorders (BD). It impacts families and healthcare professionals deeply. Family history of suicide (FHS) is one of its main risk factors, whereas lithium treatment and absence of substance use disorders (SUD) are two of its few modifiable protective factors.
ObjectivesTo explore the relationship between FHS and clinical characteristics in BD. We hypothesized that FHS would be associated with less SUD, higher rates of lithium treatment and shorter duration of untreated illness (DUI).
MethodsCross-sectional analysis of subjects with BD followed-up in a specialised outpatient unit (Barcelona, October’08-March’18). We described data with measures of frequency, central tendency and dispersion, and we used χ², Fisher’s test and t-tests for comparisons.
ResultsThe sample consisted of 83 subjects, 56.6% males, mean age 41.9 years (SD 12.7). 74.7% (n=62) had a diagnosis of BD-I and 25.3% (n=21) of BD-II. 11 subjects (13.3%) had FHS. Those with FHS did not show significant differences in sociodemographic data, DUI (58.5+/-60.4 vs 38.19+/-84.9 months, p=0.341), lithium use (72.7% vs 73.6%, p=0.95) or SUD (27.3% vs 23.6%, p=0.79). There were differences in terms of lifetime suicide attempts (54.5% vs 20.8%, p=0.026), family history of mental disorders (100% vs 69.4%, n=0.032).
ConclusionsContrary to our hypothesis, FHS was not associated with the modifiable protective factors against suicide (namely, less SUD and more lithium prescription). Similarly, we did not find an association with earlier access to mental health services at symptom onset (DUP as proxy). Therefore, our results suggest FHS does not modify attitudes towards prevention.
DisclosureNo significant relationships.
Psychiatric clinical profiles and pharmacological interactions in COVID-19 inpatients referred to a consultation liaison psychiatry unit
- N. Arbelo, M. Sagué, H. López-Pelayo, S. Madero, J. Pinzón-Espinosa, G. Anmella, S. Gomes-Da-Costa, L. Ilzarbe, C. Llach, M. Cámara, M.L. Imaz, L. Pintor
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S100
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Coronavirus Disease 2019 (COVID-19) can affect mental health in different ways. There is little research about psychiatric complications in hospitalized patients with COVID-19.
ObjectivesThe aim of the study was to describe the psychiatric clinical profile and pharmacological interactions in COVID-19 inpatients referred to a Consultation-Liaison Psychiatry (CLP) unit.
MethodsThis is a cross-sectional retrospective study, carried out at a tertiary hospital in Spain, in inpatients admitted because of COVID-19 and referred to our CLP Unit from March 17,2020 to April 28,2020. Clinical data were extracted from electronic medical records. The patients were divided in three groups depending on psychiatric diagnosis: delirium, severe mental illness (SMI) and non-severe mental illness (NSMI).
ResultsOf 71 patients included (median [ICR] age 64 [54-73] years; 70.4% male), 35.2% had a delirium, 18.3% had a SMI, and 46.5% had a NSMI. Compared to patients with delirium and NSMI, patients with SMI were younger, more likely to be institutionalized and were administered less anti-COVID19 drugs. Mortality was higher among patients with delirium (21.7%) than those with SMI (0%) or NSMI (9.45%). The rate of side effects due to interactions between anti-COVID19 and psychiatric drugs was low, mainly drowsiness (4.3%) and borderline QTc prolongation (1.5%).
ConclusionsPatients affected by SMI were more often undertreated for COVID-19. However, the rate of interactions was very low, and avoidable with a proper evaluation and drug-dose adjustment. Half of the patients with SMI were institutionalized, suggesting that living conditions in residential facilities could make them more vulnerable to infection.
DisclosureNo significant relationships.
Dhat syndrome: A case report on a culture-bound challenge
- L. Ilzarbe, D. Ilzarbe, N. Arbelo, C. Llach, G. Anmella, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S733
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dhat Syndrome is a culture-bound entity frequent in the Indian subcontinent. It is characterized by somatic symptoms, together with depressive and anxiety features, specifically focused on the belief of losing semen through urine1.
ObjectivesTo describe an atypical Dhat Syndrome case in European cultural context,and to determine the appropriate diagnostic frame and subsequent therapeutic approach.
MethodsWe present the case of a 37-year-old Indian man attended in our psychiatric outpatient unit mainly due to somatic complaints (gastrointestinal, sexual dysfunction, weakness, and dizziness). He interpreted his problem as possibly due to diabetes and hypothyroidism, and specifically from sugar loss in urine. Organic diseases were excluded.
ResultsAlthough considered as culture-bound, Dhat syndrome has been classified as a subtype of depression, anxiety disorder, somatoform disorder2,3,4, and even a prodromal phase of schizophrenia5. Antidepressants and benzodiazepines are the most recommended pharmacological treatments1. Antipsychotic agents have been used when clear psychotic symptoms were present (auditory hallucinations,delusions)5. Nonetheless, paliperidone 6mg/d was initiated at baseline, with good response and partial remission of the symptoms at two weeks, despite the absence of clear psychotic features. Culturally-informed cognitive-behavioural therapy, as well as sexual education could be beneficial were planned and initiated1.
ConclusionsData on Dhat Syndrome is scarce, yet agreement exist in considering the cultural context of the patient to avoid diagnostic delays. The adequate treatment remains uncertain. Antipsychotics may be a potential treatment. Further research is necessary to clarify the nature of this syndrome but European clinicians must be aware of culturally-mediated psychiatric manifestations which are increasingly prevalent due to globalization.
DisclosureNo significant relationships.





